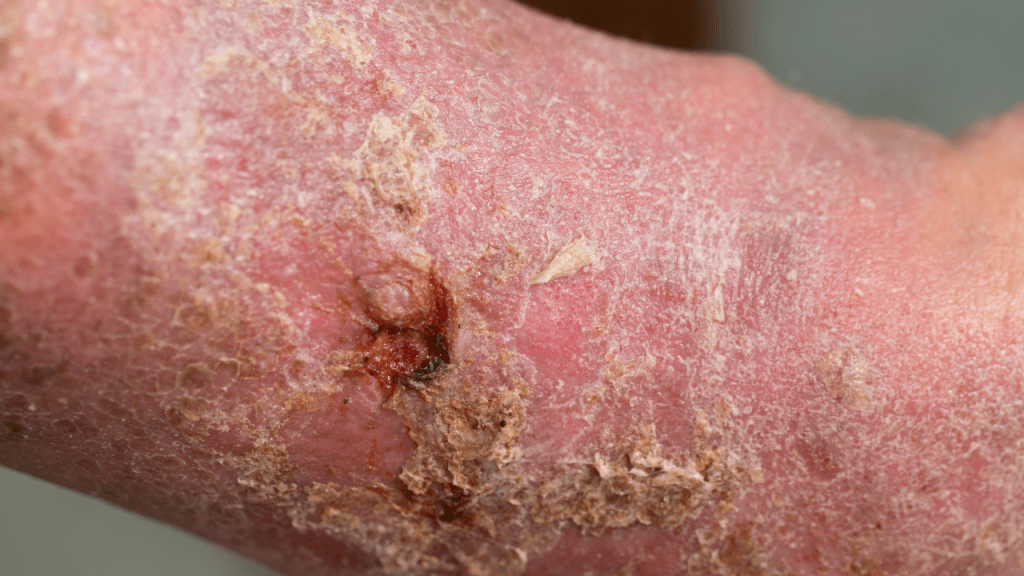
Venous stasis dermatitis happens when there’s a problem with your veins, usually in your lower legs, that keeps blood from flowing properly. As more fluid and pressures build, the blood leaks out of your veins and into your skin.
The condition is also called venous eczema or stasis dermatitis. It’s more common in people over 50. Women are more likely to have this condition than men.
Medical treatments can help, and you can do many things on your own to get the problem under control.
Symptoms OF Venous Stasis
Ankle swelling is often the first sign you’ll notice. It might get better when you sleep and then come back during the day when you’re active again. Your legs may feel heavy when standing or walking.
- The skin around or above your ankles looks reddish, yellowish, or a brown color
- Varicose veins, which look twisted, bulging, and dark purple or blue
- Itching
- Pain
- Sores that ooze, crust, or look scaly
- Thickened skin around your ankles or shins
- Hair loss on ankles or shins
What Causes Venous Stasis Dermatitis?
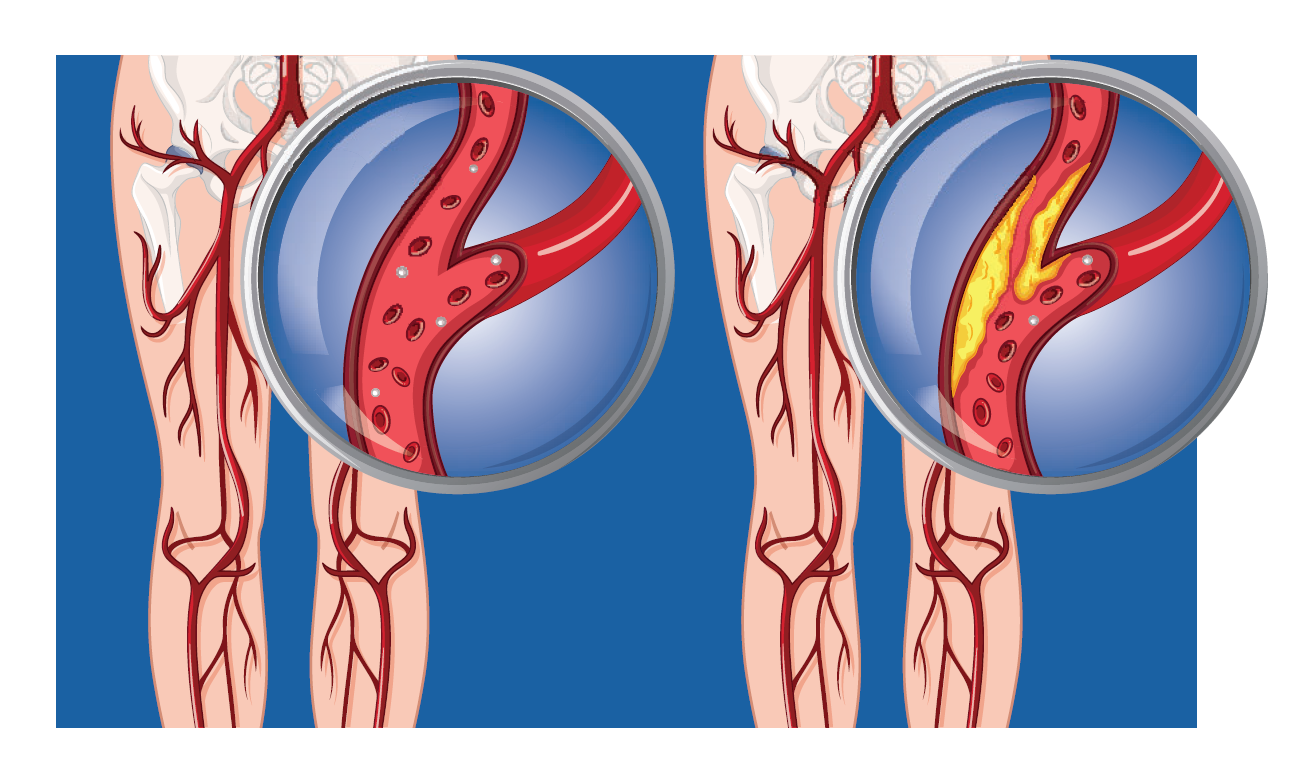
The condition often affects people who have circulation problems. When your veins don’t work well, they don’t return blood back to your heart like they’re supposed to.
The veins in your legs have one-way valves that help blood move through. Their job is to push blood up your legs. As you get older or have other health problems, the valves may not work like they should. This is called venous insufficiency.
In some cases this and other conditions can cause pressure to build. Not enough blood and oxygen reach your skin.
Some conditions that make you more likely to get venous stasis dermatitis include:
- High blood pressure
- Varicose veins
- Being very overweight
- Heart conditions such as congestive heart failure
- Kidney failure
- A blood clot, especially in your leg
- Many pregnancies
- Past surgery or injury in the area
You also may be more likely to have it if you usually stand or sit for long periods of time or you don’t get much exercise.
Treatments
Because circulation is the main cause, your doctor may suggest surgery to repair your veins. If surgery is not an option, there are other ways to get the fluid moving in your legs:
- Wear compression stockings. They can ease swelling and improve blood flow.
- Keep your feet elevated above your heart. When you can, do it for 15 minutes every 2 hours and while you sleep.
- Don’t stand in one place for long periods. Walk around often.
To treat pain, redness, or swelling, your doctor may give you a steroid or other medicine to rub on your ankles and legs. An antihistamine pill or cream might help if your legs are itchy.
You might need to wrap the area with a medicated dressing to help it heal. If you have an infection, your doctor will prescribe an antibiotic pill or cream.
A moisturizer can help with dry skin and keep the area soft. Choose one that has no fragrance, dyes, or perfumes so it doesn’t irritate your skin. Petroleum jelly and thick creams can be good options.