What are varicose and spider veins? Is each one different? What can be done to treat them? Are there any risk factors?
These are all common questions that many people have when they are experiencing varicose and spider veins.
Varicose veins, and the smaller variety known as spider veins, are abnormal, dilated blood vessels that often form in the legs. They develop when the valves of the veins weaken, allowing blood to pool in the veins. This pooling increases the pressure in the veins, and they begin to bulge or enlarge leading to varicose veins. This condition is called Chronic Venous Insufficiency.
How To Tell The Difference?
While varicose veins and spider veins have the same cause, each one is different:
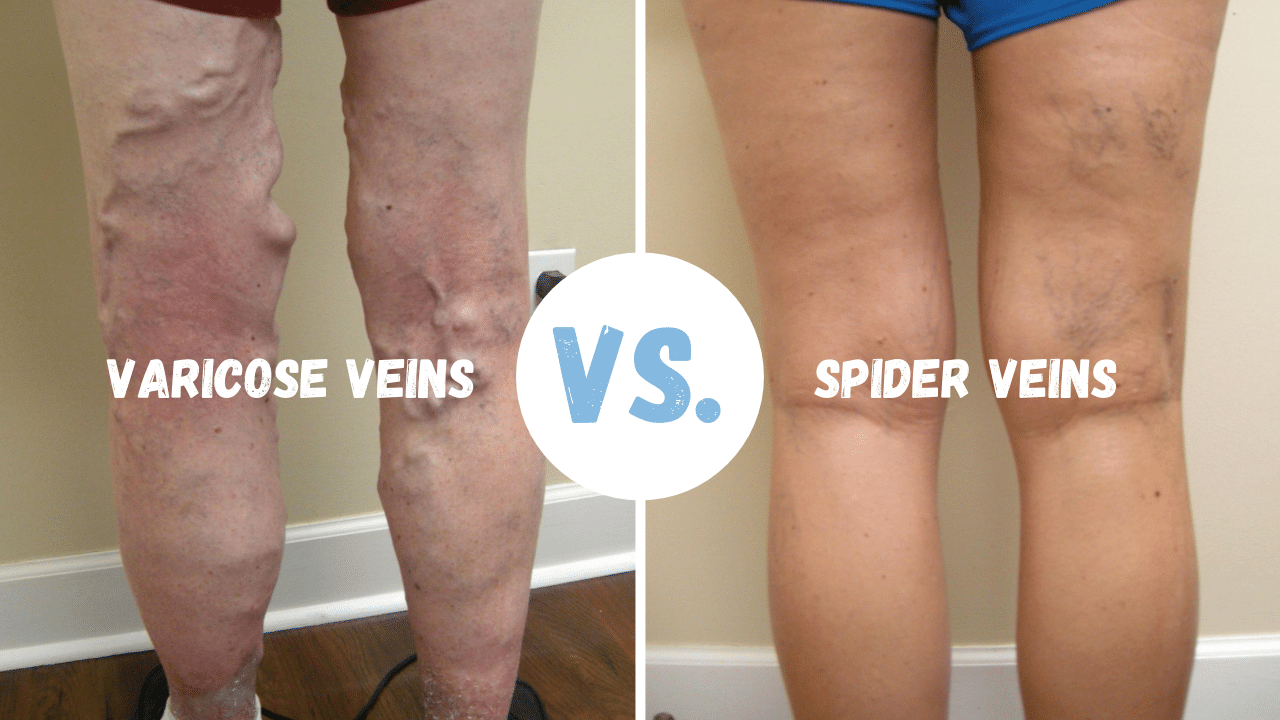
Varicose veins are twisted, bulging blue blood vessels that can be seen and felt right under the surface of the skin.
- They can cause a feeling of heaviness, discomfort, and can be painful and swell.
- They can lead to more serious health conditions such as non-healing sores and/or blood clots.
- Treatment may be necessary to prevent varicose veins from worsening and to improve how the legs look and feel.
Spider veins appear as tiny red or blue lines, usually very small in diameter, that look like branches or a spider web just below the surface of your skin.
- They’re almost always painless, do not cause leg swelling, and generally do not lead to other health problems.
- They can appear in various parts of the body such as the face, legs, and hands. The most common are leg veins.
- The cause of spider veins may not always be leaky one-way valves in the veins, they can also be caused by different forms of venous insufficiency.
- While someone can have both varicose veins and spider veins, it’s important to point out that spider veins do not always turn into varicose veins.
- Treatment of spider veins alone is usually considered cosmetic.
20 Things About Varicose and Spider Veins That You Should Know
- Very Common – About 50 to 55 percent of women and 40 to 45 percent of men in the United States suffer from some type of vein problem. Varicose veins affect over half of adults 50 years and older.
- They are not always just a cosmetic problem – they can impact how you enjoy life while possibly leading to serious health problems.
- Both varicose veins and spider veins are hereditary – if you have family members with vein issues, it’s not uncommon that you may develop them as well.
- They can be related to bodyweight – if you are overweight, you’re more likely to develop them.vi
- They’re gender-related – women are more likely to develop them than men.
- They’re age-related – as you age, varicose and spider veins are more likely to develop.v
- Pregnancy and varicose veins – but they tend to go away within 3 months after the pregnancy.
- Thought to be hormone-related – medications containing female hormones, such as birth control or hormone replacement therapy, may increase your risk of developing varicose veins.
- Your job may cause them – Do you sit or stand all day? This may worsen your varicose veins. Crossing your legs also can make them worse, as this impedes the flow of blood in your legs.
- Restless legs are a sign of varicose veins– Painful restless legs are a sign you have varicose veins. Other signs are pain while walking, feeling of heaviness, cramping, and itching.
- A vein specialist can easily diagnose your condition – sometimes a diagnosis can be made based on what you’re feeling and the physical appearance of your legs. It is best to see a specialist for this diagnosis and not your primary care physician.
- Ultrasound is the best way to look for varicose veins– this ultrasound imaging test uses sound waves to visualize the veins and measure blood flow. We offer a FREE ultrasound screening for new patients.
- Varicose veins are mainly found in the legs – but spider veins are common on both the legs, face, and hands.
- Over time, if left untreated, varicose veins can worsen and cause changes in the skin – changes might include sores that do not heal, leg ulcers, discoloration, increased leg swelling, and hardening of the skin.
- Itchy legs and ankles may not just be dry skin – varicose veins can cause itching around the ankles and lower legs.
- Varicose veins may bleed more than you might expect if injured – excess bleeding can be the result of the increased amount of blood that has pooled within the vein.
- 2-3% of people with varicose veins develop blood clots – while not as common, blood clots that form in the legs can move deeper into the veins, becoming a deep vein thrombosis, a serious condition that needs immediate medical attention.
- Lifestyle changes can improve symptoms – committing to changes in your daily life such as losing weight and elevating your legs, as well as avoiding sitting or standing for long periods, may improve your symptoms.
- Wearing Compression Stockings might help – They are often the first treatment prescribed for varicose veins.
- If lifestyle changes and compression stockings don’t help your symptoms, there are treatment options – some varicose vein treatments that can relieve symptoms and improve the look of your legs may include minimally invasive procedures, such as endovenous ablation, sclerotherapy, or microphlebectomy. Or, there are more invasive options like vein ligation and stripping surgery, which involve tying off the veins and removing them.
If you are experiencing the signs and symptoms of varicose and spider veins, you should seek the medical advice of a vein specialist. St. John Vein Center has Board Certified Vein Specialists that can properly diagnose and treat varicose veins. Our accredited vascular testing facility and highly trained staff can provide a free vein screening and evaluation, call us today (904)373-1237.