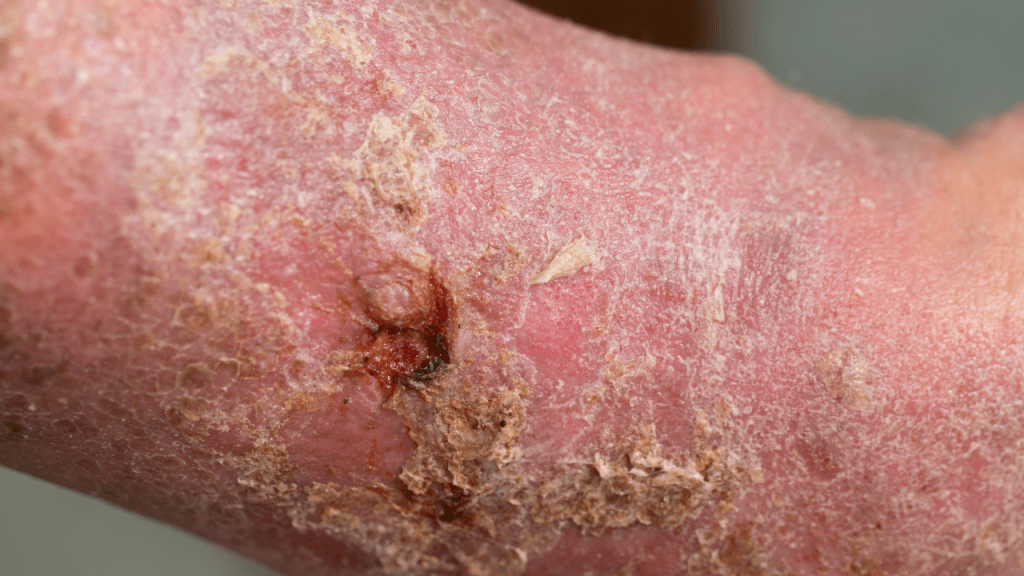
Prevent and treat venous stasis – In this interview, John Lagoutaris MD, Podiatrist at Podiatry Associates of Florida and Baptist Beaches Wound Care & Hyperbaric Medicine, reviews what you need to know to prevent and treat venous stasis.
Lagoutaris: My name is John Lagoutaris, I’m a Podiatrist in Jacksonville Beach. I work with Podiatry Associates of North Florida. We treat a number of podiatric conditions ranging from fungal nails, to bunions, to hammer toes. I’m also associated with Baptist Beaches Wound Care & Hyperbaric Medicine where I take care of podiatric conditions such as diabetic or venous stasis ulcers.
Q: What is venous stasis and how do you treat it?
Lagoutaris: Venous stasis, also known as chronic venous insufficiency is a condition of the veins. Veins are very elastic entities, they expand and contract and over time, that expansion wears out the valves that are inside the veins. As a result, blood that is getting pumped back up into the heart actually leaks down through the incompetent or damaged valves causing swelling in the lower extremities. Another cause of venous stasis is the obstruction of blood getting back to the heart, for example, blood clots. Venous stasis treatment consists of trying to control the edema, or swelling, by compression using either stockings or wraps. Other ways of treatment include exercise and staying active, elevating legs above the heart, maintain a healthy weight and quit smoking,
Q: Who is prone to venous stasis? What are the contributing factors?
Lagoutaris: Those who are prone to venous stasis are older people, overweight people, those who already have varicose veins, those who have had previous blood clots or DVTs, those with a family history of venous stasis, and people who lead a sedentary lifestyle or are inactive. If you do have varicose veins, make sure to see a vein specialist to have those taken care of.
Q: What symptoms should patients be aware of in regards to venous stasis?
Lagoutaris: The first symptom to look for is edema or swelling. If you notice swelling in your legs that was never there before, there is a chance you may be developing venous stasis. Other symptoms are tired, aching feeling in your legs, or painful varicose veins in the legs, ankles, and even feet. Some may also develop spider veins, cramping, or leg weakness.
Q: Risks of Untreated Venous Stasis
Lagoutaris: If left untreated, the ulcer could fester, become infected, and that infection can spread, not only through the body but also down into the bone. Once this happens, it increases the chance of amputation.
Q: How Long is The Treatment Process for Venous Stasis?
Lagoutaris: The length of the treatment process is completely dependent on the individual. It depends how serious the venous stasis is, on whether or not there are ulcers present. Treatment can range from a month or two to two years. Downtime is also dependent on the individual’s lifestyle and activity level.
Q: How To Control Leg & Foot Wounds
Lagoutaris: With leg and foot wounds, we want to control the edema, or the swelling, that is how these things develop. If we can control the swelling, either through compression therapy by using compression stockings or wraps then we can help to prevent or even heal these types of ulcers a lot quicker.
Q: Should I Be Wearing Compression Stockings?
Lagoutaris: I think everybody should be wearing compression stockings, but unfortunately here in Florida, the weather doesn’t cooperate very often. To answer the question of what type or what kind, I recommend you speak to your primary care physician or your vein specialist.
Q: What Are the Risks After My Venous Stasis Treatment?
Lagoutaris: After venous stasis treatment, if the edema, or swelling, continues to persist, your skin can easily break down into another ulceration. Prevention is extremely important, so: wearing your compression stockings, losing weight, staying active, not smoking, these things all play a role in preventing ulcerations.
Have you taken your FREE Personal Vein Health Assessment yet? Take it now to see if you may be at risk for venous insufficiency. Upon completion of the assessment, a member of our medical team will reach out to you via email or by phone if you prefer to review your results!